BPPV Treatment | Physiotherapy Solutions in Kellyville & Carlingford
Introduction to BPPV Treatment
Benign Paroxysmal Positional Vertigo (BPPV) is a common condition causing vertigo. However, with the right physiotherapy treatment, it can be effectively managed. At PPS Physiotherapy, we have substantial experience in BPPV treatment. As a result, we help you regain balance and confidence.
When someone experiences vertigo, their quality of life can decrease significantly. Consequently BPPV is a vestibular disorder that can lead to dizziness, unsteadiness, and balance problems. Although it is not life-threatening, BPPV can affect a person’s daily activities. If left untreated, it can cause long-term issues.
If you or someone you know is experiencing vertigo, physiotherapy can restore balance. Additionally, at PPS Physiotherapy in Kellyville and Carlingford, we treat BPPV using evidence-based methods that provide lasting relief. This blog will explain BPPV, treatments, and how physiotherapy can help you recover.
What is BPPV?

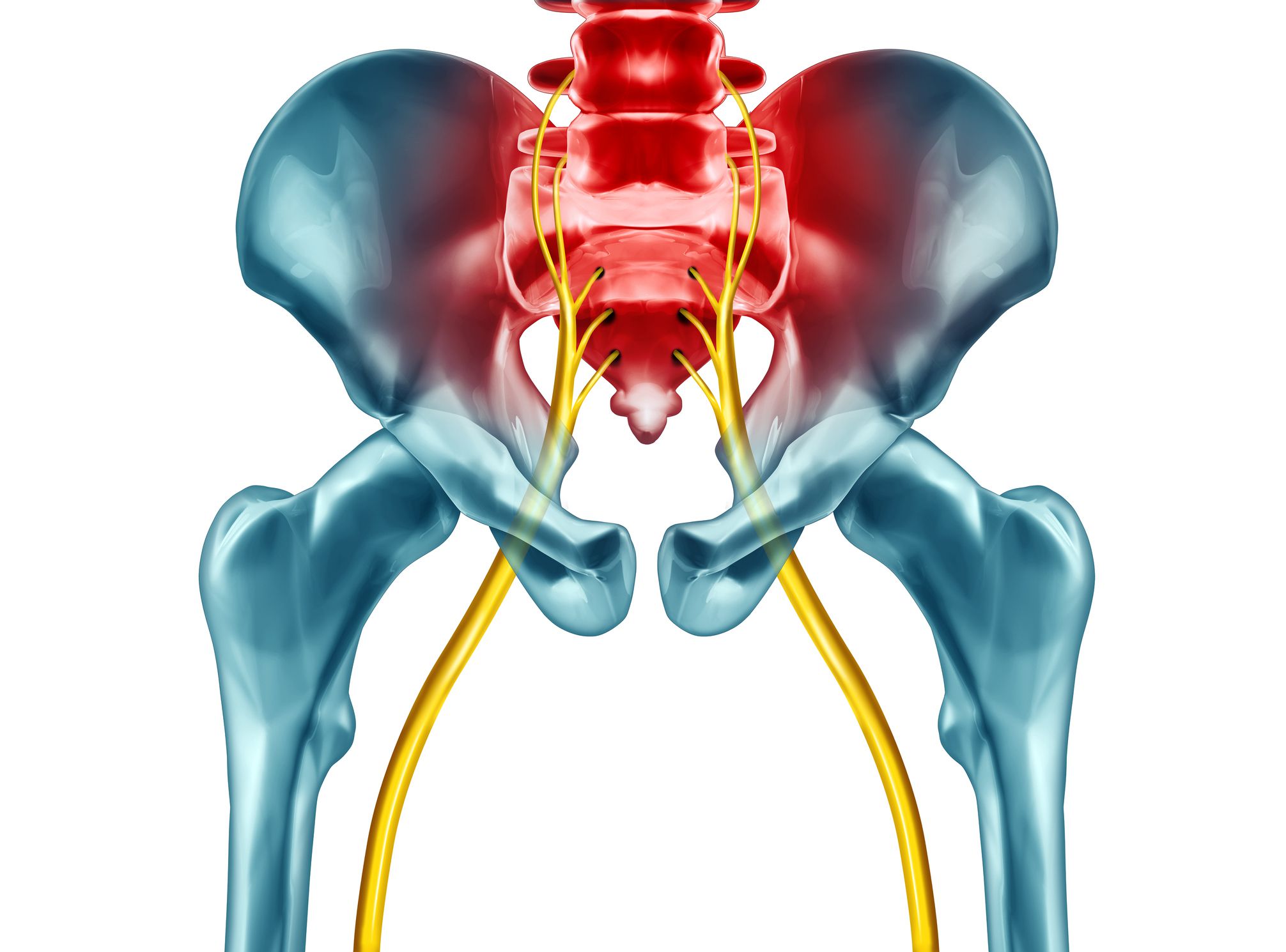
BPPV is one of the most common causes of vertigo. It happens when calcium crystals (otoconia) in the inner ear dislodge and move into the semicircular canals. As a result, this interference affects balance and causes dizziness or a spinning sensation.
Symptoms of BPPV
The hallmark symptom of BPPV is sudden vertigo. It is typically triggered by specific head movements, such as:
- Turning over in bed
- Looking up
- Bending down
- Tilting the head
These movements may cause intense dizziness or spinning. Generally, the sensation lasts for a few seconds or up to a minute. Other symptoms include:
- Loss of balance or unsteadiness
- Nausea or vomiting
- Lightheadedness
- Dizziness when looking up
If left untreated, these symptoms can worsen. Over time, the risk of falling and injury increases. Therefore, it’s important to seek treatment as early as possible.
What Causes BPPV?
The cause of BPPV is not always clear. However, there are factors that increase the risk of developing this condition:
- Aging: BPPV is more common in older adults due to the natural degeneration of the inner ear structures.
- Head injury: A blow to the head, such as a concussion, can dislodge calcium crystals in the ear.
- Inner ear infections: Infections or disorders in the vestibular system may cause BPPV.
- Prolonged bed rest: Long periods of inactivity can disrupt inner ear functions and cause vertigo.
In contrast, young people can also develop BPPV, but it is more likely to occur with age or certain medical conditions.
How Physiotherapy Can Treat BPPV
Epley Manoeuvre For Effective BPPV Treatment

The Epley manoeuvre is a common treatment for BPPV. This method involves repositioning calcium crystals in the inner ear using a series of head movements. It typically takes 10 minutes, with the following steps:
- The physiotherapist positions the patient to trigger vertigo.
- The therapist guides the patient’s head through a series of movements.
- The goal is to return the crystals to their correct location, reducing vertigo symptoms.
Semont Manoeuvre
If the Epley manoeuvre doesn’t work, the Semont manoeuvre is another treatment. This method involves quick head movements to move the displaced crystals in the opposite direction, helping restore balance.
Brandt-Daroff Exercises for Vertigo Relief

Brandt-Daroff exercises help patients manage vertigo at home. These exercises allow the brain to adapt to dizziness, reducing vertigo symptoms. Physiotherapists often recommend these exercises for patients who have mild BPPV or after the Epley manoeuvre.
Why Choose PPS Physiotherapy for BPPV Treatment?
- Experience and Knowledge: Our physiotherapists have years of experience treating BPPV and other vestibular disorders. They perform thorough assessments and deliver effective treatments for vertigo and balance issues.
- Evidence-Based Approach: We use proven techniques like the Epley and Semont manoeuvres. These methods are based on the latest research, ensuring high-quality care for our patients.
- Personalised Care Plans: We create individualised treatment plans based on each patient’s unique condition. This approach helps patients regain balance and confidence.
- Convenient Locations: Our clinics in Kellyville and Carlingford are easily accessible, providing ongoing care for BPPV and other conditions.
Contact PPS Physiotherapy Today
If you have BPPV, physiotherapy offers a safe, effective solution. Our team at PPS Physiotherapy can treat BPPV with proven methods. Whether you’re ready to regain your independence or improve your balance, we can help.
Contact us today to schedule your appointment and take the first step towards a vertigo-free life!
Helpful Resources:
Learn more about vertigo treatment from the Australian Government’s health department.
Journal of Vestibular Research – Consensus on BPPV






 \
\