For alot of our amateur athletes the off-season is a time for resting and enjoying the weekends before winter sport starts up again in March/April. For most people this means they have 5 or so months off each year from their chosen sport. This time might be spent doing nothing at all, pursuing a different sport or engaging in a different type of exercise.
The golden question is what is the best way to spend your off-season? You want to find a balance between rest and recovery but at the same time don’t want to lose all your fitness. Easier said than done for your average joe blow who doesn’t have the help of a strength and conditioning coach to guide you through the process.
Hopefully this blog helps to shed some light on how you can achieve that balance and plan out your own off-season!
What is the off-season?
For every sport there is a designated period of time where the season starts and ends. Outside of this competition period is termed the off-season. The off-season first and foremost is a time for physical and mental recovery which is important to avoid overload and burnout. It’s all about RELATIVE REST though! The off-season shouldn’t be a ticket to do nothing for weeks on end. The second focus of the off-season is to work on sports specific skills that you need to improve on, strengthening any week points in your physical or mental game, working to resolve any injuries that have been niggling and addressing any deficits that may assist in injury prevention.


Physical and Mental Recovery
After a long season both the body and mind needs time to recover and replenish. If you neglect taking time to rest you may increase your risk of injury. As mentioned before, relative rest or active rest is a good way of looking at this. You don’t want to do absolutely nothing but instead of running like you would during the in-season try some lower impact exercise instead eg. cycling or swimming. Changing the type of exercise you are doing can also be beneficial for mental recovery. If you do the same type of exercise and training all year round you may start to feel stale and burnt out from the repetitiveness.
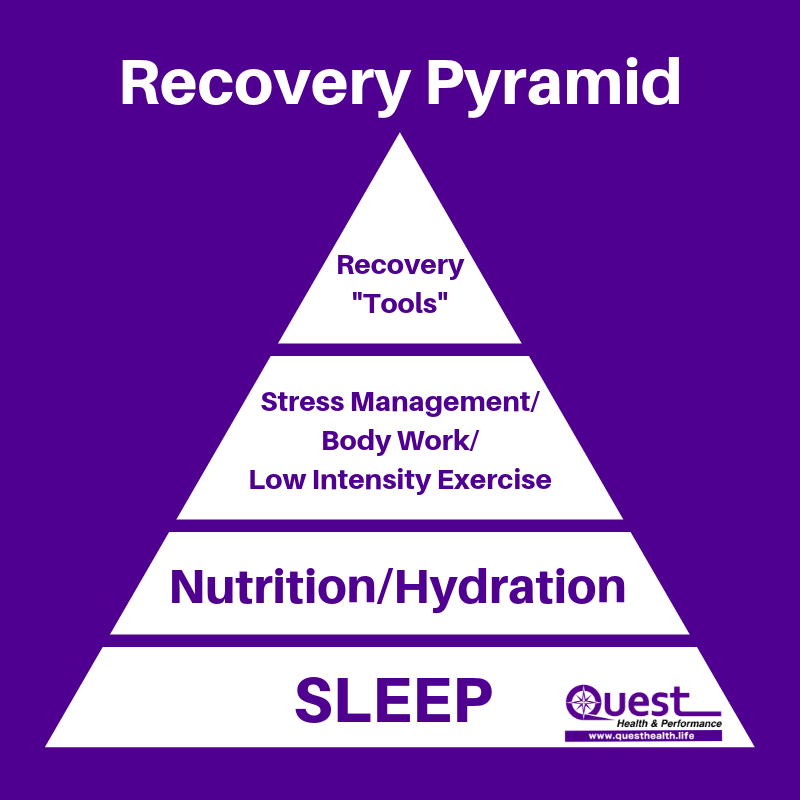
You may also want to use the 100 point recovery system which is a great tool for both in season and off-season. The recovery tool ensures you are are dedicating enough time to your recovery which will in turn assist with optimising your performance and decreasing injury risk. You can choose from different activities to accumulate 100 points of recovery. There are a few different versions available online or you may have one you have used previously.

Addressing Weaknesses
If you have found that there is an area of your performance that has been suboptimal over the past season, now is a great time to work on it. This may look like addressing a strength discrepancy between limbs, improving a specific skill or improving your your ability to generate power. Whatever seems to be the hole in your game take time to work on it!
We know that for certain sports, weaknesses in some muscle groups or movement patterns are high risk for developing an injury.
For example;
- Netball – having suboptimal landing strategies can predict those at risk of sustaining an ACL injury
- Soccer – having weakness of the adductors (groin muscles) can lead to adductor related injury
The key to working on these in the off-season is that practice should be done that is very specific and not with the same intensity or frequency as in season practice. Remember we are finding a balance between active rest, recovery and getting to work on our weaknesses. It would be best to work with a coach who knows you and your sport to identify what specific areas you need to work on.
Why should I exercise in my off-season?
The off-season is one of the most important phases of the year. It is the time that prepares you physically and mentally for what’s to come over the subsequent 6-9 months. The competitive season is often long and you don’t want to break down half way through.
- Aerobic Preparedness – As much as you are actively resting and will likely lose some aerobic conditioning it is much easier to build up from 60% of your max (40% loss with active rest) than it is from 30% with complete rest. When we remove the physiological adaptations of training that you were used to, the body undergoes a deconditioning or reversal response. Our fitness is a use it or lose it principle so the body will de-train when we don’t apply the same stimulus. It is very normal and quite ok to experience some aerobic deconditioning. However, you would rather lose a modest amount opposed to alot to make returning to pre-season much easier.
- Tissue Preparedness – Similar to aerobic preparedness, our tissues undergo a de-training effect when we remove the stimulus of training and competition. Tissues, such as our tendons, are very load tolerant structures and they like to do the same amount of load week in and week out. They don’t like rapid increases in load and if this happens you may develop tendon pathology. Again, it’s ok to lose some tissue capacity but its much easier to build back up in the pre-season if you have been doing active recovery than it is from 3 months of complete inactivity.
- Injury Prevention – As previously mentioned injury prevention is a big one! The pre-season training block is often not enough time to work on any imbalances from the prior year, hone in on improving specific skills, increase your aerobic and tissue capacity back to in season levels, return to game simulation, learn new skills/formations and get used to playing with a new team. It’s just not practical! Additionally, if you do stop completely over the off-season you will likely have to increase your loading massively week to week to be fit and ready. We know that rapid increases in load are a strong predictor for injury and you will likely be seeing a physio before your season even starts.

- Mental Health – Exercise and physical activity has time and time again proven to be a great support for our mental health. Going from being in season, training and competing with a regular routine to no structured exercise can wreak havoc on you mentally. A simple walk each day can help you clear your mind, get some fresh air and improve your mental health. You may also find it helpful to keep some form of loose routine if you are someone who is very routine orientated.
If you are entering the off-season of your sport now is the time to start planning what the next 6 weeks to few months is going to look like. If you need help working out what you should be working on then speak to your coach or a physiotherapist for a personalised injury prevention plan. Our friendly team of physio’s are all experienced sports people themselves and have a diverse knowledge of the demands of sport. Call our reception team today on 9672 6752 (Kellyville) or 9871 2022 (Carlingford) to book an appointment.
Kimberley Cochrane – Physiotherapist (Bachelor of Physiotherapy, First Class Hons; Grad Cert Sports Physio)



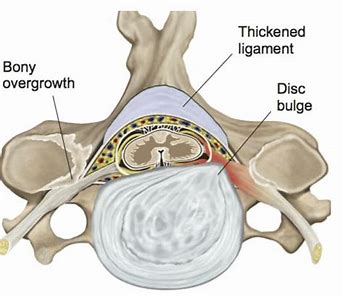





 Overhead activities
Overhead activities