It’s been a difficult past couple of years as we’ve struggled through the global pandemic of Covid-19. As cases, hospitalisations, and deaths continue to rise it’s easy to feel anxious about whether or not you, your family or friends will be hit by the virus and what will happen to you if you do get it. The vaccine program has offered some hope and re-assurance that whilst we may still contract Covid-19 we are far less likely to be severely ill or die as a result. However, the more actions we can take to reduce our chances of becoming severely sick the better.
One of the easiest ways to reduce the severity of illness is by keeping active and regularly exercising. The British Journal of Sports Medicine has published a study with over 48,000 participants demonstrating that regular physical activity is able to greatly reduce the likelihood of severe symptoms, the rate of hospitalisation, and the rate of death from Covid-19. There are many uncontrollable risk factors which may increase your risk of severe Covid-19 including older age and underlying health conditions. However, whether or not you are physically active is one that you are in control of and can change!
Before you decide to go and start a 6 day gym routine, the positive impact exercise has on reducing morbidity and mortality from Covid can be observed with even small amounts of physical activity. This means, if you are not doing any exercise at all, starting even a modest amount can offer great additional protection. It is widely known that physical activity has a broad range of health benefits including weight management, improved mental health and reduced risk of lifelong illnesses. By getting active, it also helps to improve your immune function, heart health, lung health, and increases the strength in your arms, legs and torso.
How much should you be exercising?
The World Health Organisation (WHO) recommends adults should be doing at least 150–300 minutes of moderate physical activity per week or at least 75-150 minutes of high intensity exercise a week. They should also do muscle-strengthening exercises that involve all major muscle groups on 2 or more days a week, as these provide additional health benefits.

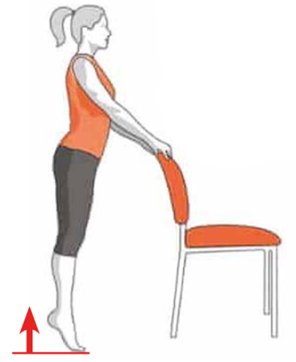
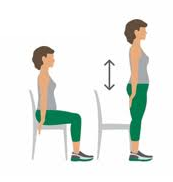
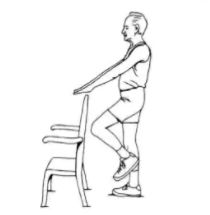
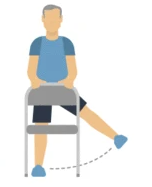
Physical activity plays a huge role in reducing the severity of many diseases (not just Covid-19) and we should all be participating regardless of whether we have been affected by the virus or not. Physical activity does not mean you have to be running for hours in the park or playing club football. It can be any activity that requires you to get your body moving and using some energy. During this lockdown it’s been very difficult to stay active with the closure of gyms, trying to keep our distance from others, and finding the motivation to get up off the couch. Popular ways to participate in some physical activity during COVID-19 include walking, cycling, playing with your family, and participating in some recreational sports. These can be done at any level of skill and it should be enjoyable for all.

The evidence is there that physical activity needs to be a priority in our day especially during the pandemic. It keeps our body and our mind healthy and as stated previously, it has a role in limiting the adverse effects of COVID-19.
We hope you’re all staying safe and well.
Sincerely,
PPS Physiotherapy family