Playing sport comes with an inherent risk of injury. As much as we would love to prevent major injury unfortunately at times they are inevitable.
Suffering an ACL injury can be season ending. For many years surgery surgery has been a pre-determined sequalae post ACL injury. However our ever evolving world of research is starting to change this trend.
What and where is my ACL?
The Anterior Cruciate Ligament (ACL) is located deep inside the knee joint and forms a cross with its closely related partner the posterior cruciate ligament. Ligaments in general function to increase stability and control joint motion. Thus, when there is no ACL certain motions are unrestricted and more movement in the joint can be elicited. This can make the knee joint unstable especially during rotation or landing movements.

How can you injure your ACL?
ACL injuries can be broadly classified into contact and non contact injuries. Contact injuries occur when something external causes you to lose balance/twist/fall which results in damage to the ligament. This is in contrast to a non contact ACL injury where you were solely in control and the ACL ruptured. The mechanism of injury that triggered your ACL defect is actually really important for your physiotherapist to know as we manage them slightly differently.
ACL injuries are common in sports requiring pivoting, cutting/change of direction, jumping/landing and contact situations. Thus high risk sports include; netball, basketball, soccer, tennis, touch football, oz-tag, rugby league and union and soccer. That is not to say that you won’t injure your ACL doing another activity it is just less likley. In fact we had a patient attend our clinic who stated “I was just running in a straight line and my knee gave way”. This ended up being a complete non contact ACL rupture…this mechanism is by no means common so don’t go giving up on your running program just yet.
Can I prevent ACL injury?
YES, YES, YES!!! Prevention is the best option for reducing your risk of injury. Prevention should start with children commencing their first season of sport and continue throughout life. The same rule applies for adults returning to sport or continuing to play. In recent years some great ACL prevention programs have been developed by Netball Australia and FIFA. The Netball KNEE program has multiple different levels of play and ages so can be tailored to any individual. You can obtain a free copy of the program from the link below.
https://knee.netball.com.au/

The aforementioned programs are heavily geared around preventative exercises which are gold standard practice in injury prevention. However, purchasing correct fitting and sports specific footwear may also help to reduce your risk.
What do I do if I sustain an ACL injury?
In most cases there will be a sudden event in which you may hear or feel a crack, pop or snap followed by pain. The knee will swell up quickly however you may still be able to weight bear on it. If you suspect you have sustained an ACL injury but are unsure you can attend your physiotherapist for evaluation. If they suspect an ACL or meniscus injury they may refer you for an MRI to confirm the extent of the injury. You could also attend your GP who can assess the knee and refer on for imaging.
As soon as the injury has occurred apply ice and elevate the leg to settle both the pain and swelling. If you have a tubigrip (a tight stocking like tube of material) apply it to the knee for some compression.
My ACL is partially torn what now?
Partial tears can definitely occur and can be difficult to detect without MRI. Once this has been determined physiotherapy aims to maintain muscle strength, muscle mass, cardiovascular fitness, proprioception and stability without further stressing the ligament. Depending on the severity of the strain you could expect up to 12 weeks off sport. Partial tears rarely require surgery unless they progress to a full tear.
What about a complete ACL tear what are my options?
So this is where it gets interesting! As mentioned before, in recent years research has started to suggest not everyone needs an ACL reconstructive surgery. There are 2 types of people post ACL injury; copers and non copers. Copers can be classified as people who have good knee stability and are able to compensate after injury whereas non copers experience ongoing instability and little to no compensation. Which category you fall into can really only be determined after 3 months of rehabilitation/prehabilitation.
After this 3 months a mini assessment should be conducted, your results discussed with you and a decision made to continue conservatively or to seek a surgical opinion.
- Surgery
If you opt for surgical reconstruction you should be aware that the rehabilitation time is usually 12 months. Surgical intervention comes with significant costs (time, financial) and does not guarantee that you won’t rupture the same ACL (now a graft) down the track/when you go back to sport. In fact this trend has been on the rise over the last few years. There can also be complications of surgery such as DVT, cyclopse lesion, issues with the pins or graft itself. Most surgeries will go uneventfully however risk of re-rupture, especially in an adolescent age group is quite high.
Considerations for choosing surgical or conservative management should account for the following;
- Has the person done 3 months of high quality rehab?
- Does the person fall into the copers or non copers group?
- How stable is the knee joint functionally?
- What sport does the person play?
- Does this sport require alot of rotation, pivoting and landing and how stable is the knee under these conditions?
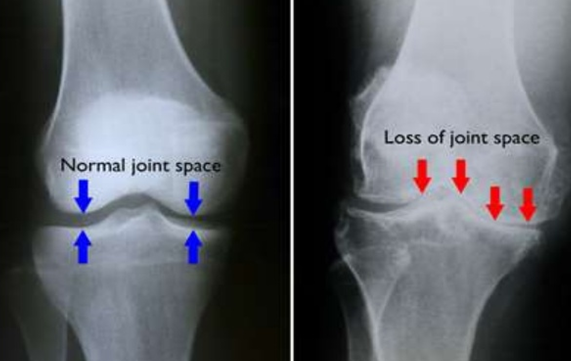
- How old is the person and is there any degeneration already occurring in the joint space?
Note: Just because you play a pivoting sport doesn’t mean you will have to have an ACL reconstruction!!! It is all about how well you can compensate for the deficit.

2. Conservative
For some people conservative management is a better choice or may even been an interim choice. 3 months of conservative physio may be recommended to determine if you will fall into the coper or non coper group. This period of time may also be used as prehabilitation. Prehabilitation refers to undertaking a rehabilitation period prior to intervention on the premise the better you go into surgery the better you come out of it. Once we sustain an injury and experience pain around the site we can get what we call muscle inhibition (basically where the muscles don’t activate how they should). This can lead to significant muscle weakness and atrophy if its not addressed.
For some people surgical intervention may not be appropriate. One such group are people with osteoarthritic change (usually 50+) where surgical intervention may rapidly increase the rate of osteoarthritis in the knee. These people should be managed conservatively where possible. An old school train of thought is that without the ACL there will be increased movement in the joint and an accelerated degeneration process. This is in fact false and providing you fall into the copers group there is no reason why you can’t function highly without and intact ACL.
It is important to recognise that an isolated ACL injury is not a medical emergency. You DO NOT need to have surgery the same day or in the following days after injury. You might want to take some time to weigh up your options and discuss with a physiotherapist your thoughts as well as seek advice.
If you have any questions regarding ACL ruptures and management, feel free to ask one of our physiotherapists. For bookings please call 9672 6752 (Kellyville) or 9871 2022 (Carlingford).